Erik had been in cardiac ICU for days. He was on the transplant list at Status 1A which meant he required two intravenous drugs around the clock and doctors had given him less than 20 days to live without a heart transplant. It had been almost 40 days.
Waiting on a heart for a man who is 6’4″ 200 lbs. is typically a longer wait than for a woman or smaller man. A heart recipient can take a heart that is too big, but not one that is too small. So we were waiting on a very specific sized heart in Erik’s case.
He had not left the 6th floor at St. Paul Hospital in Dallas since April 16. We had enjoyed some short spurts of time in a regular room, but he had been in and out of ICU for months as his condition deteriorated.
June 15th was Father’s Day. Bryce and Lexi (ages 6 and 4) came from Tahoka with my parents and had spent a couple of days hugging on their dad when they could. When it was time to leave, Bryce would not…..could not let go of Erik. He cried and cried for really the first time and was not ready to leave. Mom and Dad and I finally coaxed him into the car and they pulled out of that parking lot with my 6 year old baby looking out the back window, sobbing uncontrollable tears. That little broken heart just killed me. I walked back inside, swallowed the huge lump in my throat and sat down in the ICU waiting room to eat an entire carton of mint chocolate chip ice cream. It was all about survival.
Later that afternoon we got a visit from one of the heart surgeons on Erik’s transplant team. He told us the team had decided that the very next day they would need to conduct open heart surgery and implant a left-ventricular assist device (LVAD) into Erik’s abdomen to help his heart pump. He said Erik would not live through the week without it. We could not wait another day for a heart. This possibility had been mentioned by the doctors, but obviously was not the best case scenario. For one thing, anytime you have surgery there is a risk of infection. If this were to happen Erik would become ineligible for a transplant should a heart become available. And two, this was major open heart surgery on Erik’s poor body which was already so weak and frail. The risk of death on the table was another real factor we had to consider. But ultimately, there was no choice.
The rest of that Father’s Day I spent getting educated on the LVAD and what it would mean for Erik as he waited on a transplant. Once Erik recovered from the LVAD implantation, we would be able to leave the hospital and go as far as Frisco to live with my sister and her husband. He would remain on the transplant list, but would be moved to status 2 which meant he would be lower on the list – not ideal, but at least he would be out of the hospital.
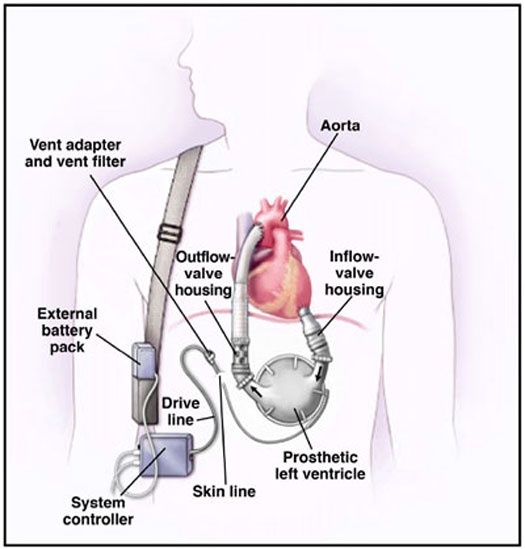
The first generation LVAD was a 3-pound pump which they explained would be connected to Erik’s heart to help the weakened ventricle pump blood throughout the body. Cords would come out of his abdomen and literally plug into a battery pack or a wall outlet. Erik’s sister Aleisha, my sister Kelly and her husband Matt would all join me in a 12-day training class to learn how to keep the batteries charged, how to manually pump the LVAD in case of a power outage and how to handle an emergency situation if the pump failed. Our transplant coordinator, Katy, visited the Frisco fire department near Kelly’s house to give them first aid training in case they ever received a 911 call from Kelly’s house. Also, I would be in charge of his sterile dressing changes – an adventure in itself.
The LVAD of today is much smaller and operates completely differently. The patient has no blood pressure and no pulse. And there are no exterior cords. The folks who receive LVADs today have no idea what past generations of patients had to go through. Erik’s pump was gigantic and loud and invasive. To say the least.
Left Ventricular Assist Device – First Generation
As I began to understand what was about to happen, I can remember looking around and thinking, where are the grown-ups? I was only 30 years old and could not imagine that I was the responsible party in all of this. Shouldn’t an actual adult be in charge here?
Monday, June 16, 2003.
Early Monday morning, Erik underwent his first open heart surgery. It lasted about 6 hours and he did remarkably well. There were no complications.
I sat with him the rest of the night in ICU as he slept, then returned to my little private room in the guest house attached to St. Paul. As always, I slept hard. God blessed me with good sleep in the hospital for all those months. I don’t remember praying for that specifically, but He was so good to me and so generous with rest. I’m so thankful.
The next morning I tiptoed into ICU as early as I could and found Erik sitting up in the chair watching television. I was first struck by the sound of the machine where the batteries whirred. Then the sound of the pump took my breath away. No words can convey the look on Erik’s face – he looked shell shocked, surprised, terrified. He had woken up to cords coming out of his body and he was attached to a machine about the size of a large bookcase. And the nurses had gotten him out of bed and guided him into the chair. I covered my mouth to stifle the cry. To this day I believe Erik suffered from some form of PTSD because this implant was physically devastating. But he never complained even for a moment.
Later that day, Erik admitted that he could actually see better than the day before, and his hands and feet were no longer like icicles since the blood was finally circulating into all the extremities. The LVAD had already improved his quality of life, even though in itself it was a monstrosity.
The next few days are a blur. I got trained on the sterile dressing changes and we all started our daily classes on the LVAD training. We sat at the round table in the hospital conference room with Katy, the transplant coordinator. And Erik sat next to us on the couch. Sitting straight up, he would doze in and out of sleep and then jerk awake periodically. When your eyes are closed do you ever imagine a basketball coming right for your face and it makes you jump? Erik started doing that after the LVAD and still does it when he sleeps. I think it’s just another result of this surgery and the trauma it caused him. Bless him.
Tuesday, July 1, 2003
The day finally arrived when Erik was recovered enough to be released from the hospital. I packed up four months’ worth of magazines and get well cards and started loading the car to head to Frisco. Kelly, Matt and I felt ready to handle any emergency and were just eager to get him home. We planned our first dinner out to Macaroni Grill with Aleisha, Sarabeth and Amanda.
It was quite a sight seeing Erik walk into a restaurant for the first time in months. Every head would turn and people would stare at the battery pack and wonder what in the world the sound was. I just smiled and felt the need to mention to almost everyone that my husband had open heart surgery a mere 15 days prior. (This was an urge I experienced for a long time and Erik finally made me stop doing it from sheer mortification. I believe the term is “TMI”.)
We sat in Matt and Kelly’s living room for hours that day watching Rachael Ray’s cooking show. It felt so good to sit next to Erik on a couch outside of the hospital.
The next day I did my first solo sterile dressing change which involved meticulous hand washing, and the use of a sterile field and gloves to replace all of Erik’s bandages. It was also very emotional for me as I cried trying not to hurt him, gently wiping away blood and applying alcohol to the 5 exit wounds. What precious, intimate moments Erik and I shared as he laid still reassuring me that he was fine and hardly flinching at what must have been intense pain. I was scared to death I might accidentally contaminate the field, but I would not have traded that job with any other soul.
The rest of the day we spent running a few errands and just enjoying being together. I had to drive everywhere (slowly and gently) and Erik had to sit in the backseat bravely surviving one unfortunate incident with a curb. I still feel bad about that. Other than the batteries and the bandages everything felt almost normal.
Thursday, July 3, 2003
Less than 48 hours later, at 5:16 a.m. Kelly and Matt’s house phone rang. I picked up the phone at the same time Matt did and I heard the voice of one of our transplant coordinators. Kathy said, “Matt, I need you to wake up Erik and Jennie. We think we have a heart.” I told Kathy I was on the line and she continued, “Please do not speed or take any risks getting here, but we do need you to hurry.”
My heart is pounding just writing about this moment….it was surreal. The whole time Kathy was talking, I was shaking Erik’s shoulder to wake him up. As soon as I hung up the phone, that house lit up and became frantic and crazy. Erik sat on the bed while Kelly, Matt and I rushed around brushing our teeth and putting on shoes. Kelly said she would stay behind to let the dog out and to blow dry her bangs (This is a real problem for Wells girls. The struggle is real.)
So Matt and I gently helped Erik into the backseat then jumped in the front seat of his car. I began making calls to our parents and a couple of friends in Lubbock who could spread the news. In the meantime, Matt chose his route to the hospital and then we argued the entire way because I disagreed with the highway he took. Occasionally Erik would say from the backseat, “Really, ya’ll are doing this now?”
We finally pulled into St. Paul’s driveway and Kelly had beaten us there! Along with Aleisha, Sarabeth and Amanda who had all received phone calls from me as we left the house. Do you think for a moment I have ever let Matt forget this? You know me too well.
What can I say about transplant day? The mood was celebratory. We went straight to the ICU and Erik entertained us with his imitation of showing pigs. Imagine his frail little body with cords and batteries all over him, squatted down with his hand out like he was showing a pig in a stock show. The rest of us were on the floor laughing with tears streaming down our faces. I still can’t believe he was so energetic and care-free that morning.
It was still dark when they came to take him back to surgery. Dr. Montcrief shared the only details he could about the heart Erik was about to receive; it was young, athletic and healthy. Erik and I held hands until the elevator closed. And then I fell into my sister’s arms and cried.
Our family filled up the waiting room that day. There were 18 of us eating bagels and waiting as patiently as possible. At some point I realized I still had on pajama pants and the ratty t-shirt I had slept in. Thankfully, the guest house still had my old room available so I ran to shower and put on clothes – the fastest 15 minutes of my life.
Back in the waiting room I would periodically get a call from the operating room. One of the nurse practitioners I had become friends with was allowed to observe the surgery so she was put in charge of providing me updates. She called first to tell me that Erik was on bypass. Then she called again to tell me the new heart had arrived. Later she called to tell me they were removing Erik’s heart and she described what it looked like – grey, shriveled and not really beating. It just kind of quivered.
After about 7 hours, I was informed that Erik was headed to recovery and that the surgery had gone perfectly. The LVAD was gone and Erik had a new heart. The sigh of relief in the waiting room might have been heard from miles around, as we all packed up our things and headed to recovery.
Erik was in ICU for a couple of days and then moved to a regular room on the 6th floor. He began his large regimen of medications which he still takes – 42 pills daily. And he can take them with a tiny sip of water which never ceases to amaze me and the kids.
Living on the transplant floor we met numerous families on similar journeys and we found that most times, a transplant patient might remain hospitalized anywhere from a month to 3 months after transplant just trying to get their medication straightened out. And many times after being released, a transplant recipient would come back into the hospital due to rejection or infection.
Erik was released from St. Paul 11 days after transplant with no sign of rejection. His blood work and vitals were perfect. Can you believe that? And other than one harrowing experience a couple of weeks later, Erik stayed healthy and never got readmitted. (I wrote about that a few years ago.)
hems of my HEART
There are countless other stories about things that happened to us in the hospital during the weary months of 2003 – such as going to battle with the hospital administration which wanted to reject our $250,000 insurance policy because that wouldn’t be enough and his transplant was elective; and the verbal beat down I gave a priest who walked into Erik’s room and asked what sin he had committed to bring this illness on himself; and the fact that every night I slept in the guest house I could hear it raining, even though it never rained.
Erik had the LVAD for 2 ½ weeks before his transplant, so I will always wonder what the last two weeks of our heart donor’s life were like. I like to think they were profound days where he got to see some special people for the last time or God finished a precious work in him. We will probably never know. Erik has never struggled with guilt of any kind, because why would he? He did not cause the death of an 19-year-old kid, but because of a mother’s selfless decision to donate a heart, Erik got to live. We are just so thankful.
I’m overwhelmed with gratefulness that Erik has been so healthy for the last 12 years. He’s surpassed most expectations and continues to impress his doctors with his healthy kidney and liver functions, as well as a heart that has never rejected. I have every reason to believe that he will be around to walk his daughters down the aisle and even meet his grandchildren. That is our prayer.
God has always gone before us. He hems us in, behind us and before us. He has granted peace in the storm and wisdom in the darkness. He continues to favor Erik’s health and I believe it’s because of the thousands of prayers on his behalf all those many years ago, as well as today.
Thank you for letting me share our journey. Many people reading this walked this path with us 12 years ago. You loved us, you loved Bryce and Lexi, you helped our parents, you packed boxes and moved us out of our rent house into storage, you donated money, you fasted, you prayed, you wore out the carpet in your house pacing back and forth in earnest prayer for us.
How can we ever truly say thank you? The communion of saints is something to behold and I love every one of you. Blessings, Jennie



Tears again. I'm glad you share. Via Abby I prayed through that time for you all and it is meaningful to see how it all worked out from the inside out. Thanks to your experience I have learned how meaningful and valuable donation is.
LikeLike